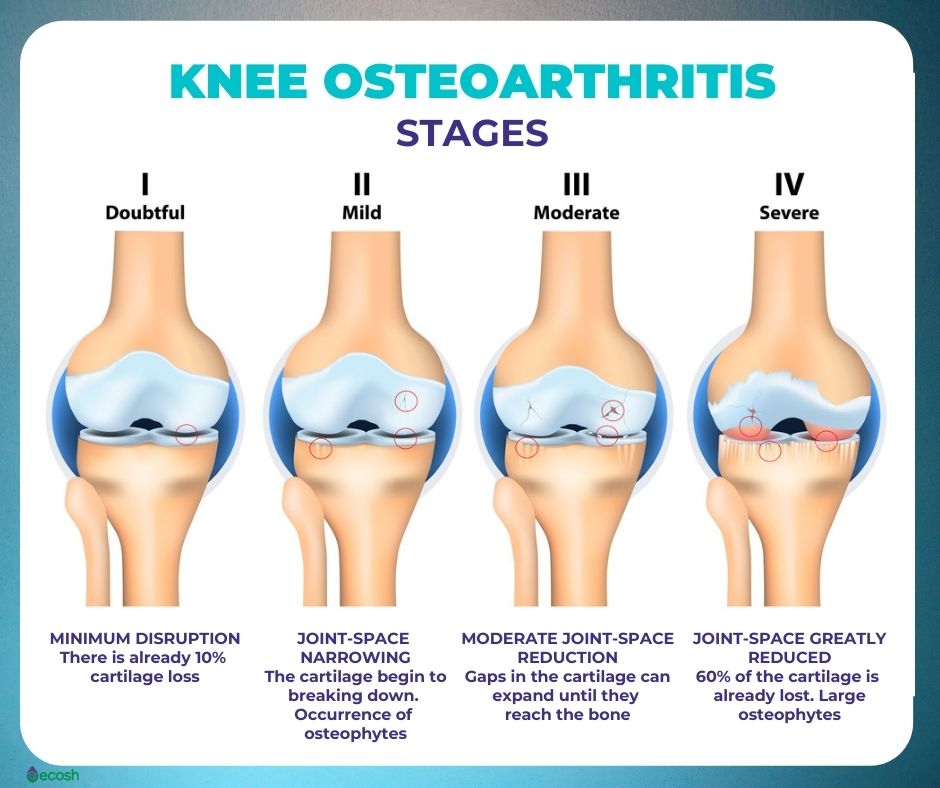
Osteoarthritis is the most common form of arthritis that happens when the cartilage that cushions the ends of bones in your joints gradually degenerates – meaning, it wears down over time.
Cartilage is a dense and slippery tissue that enables untroubled joint movement. Finally, in case osteoarthritis, if the cartilage wears down entirely, bone will rub on bone.
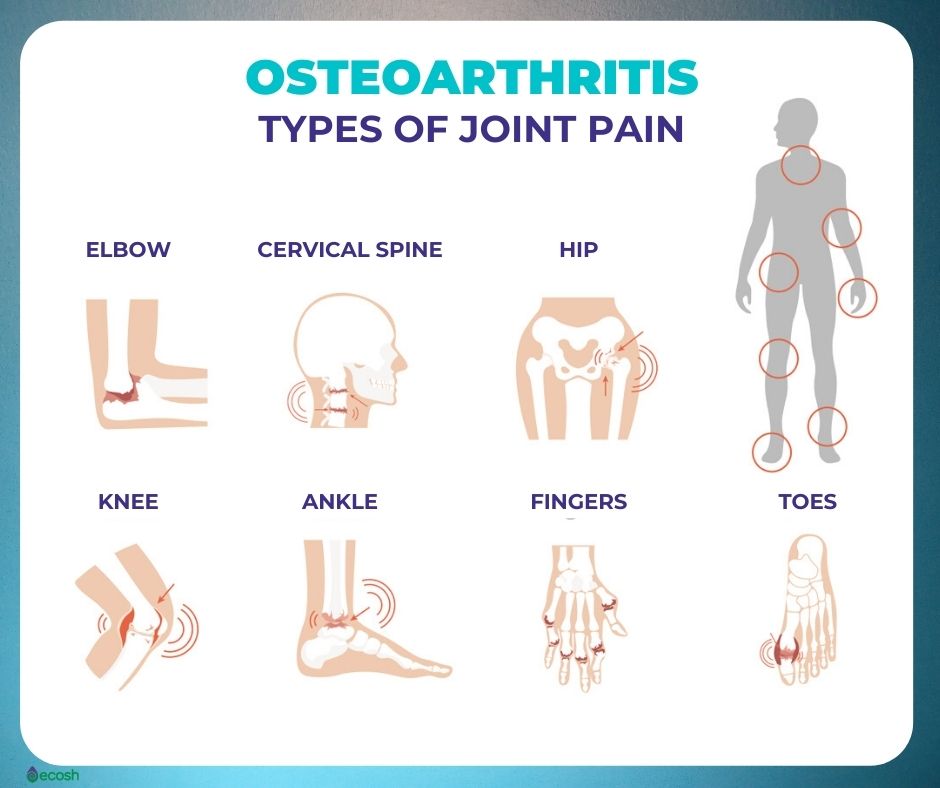
Osteoarthritis can affect any joint, however, the disorder usually damages joints in your knees, hands, spine, and hips.
Osteoarthritis can`t be reversed, however, the symptoms are usually manageable. Maintaining a normal weight, staying active, healthy diet, some conventional and home treatments might slow progression of the disease, relieve pain and help improve joint function (1).
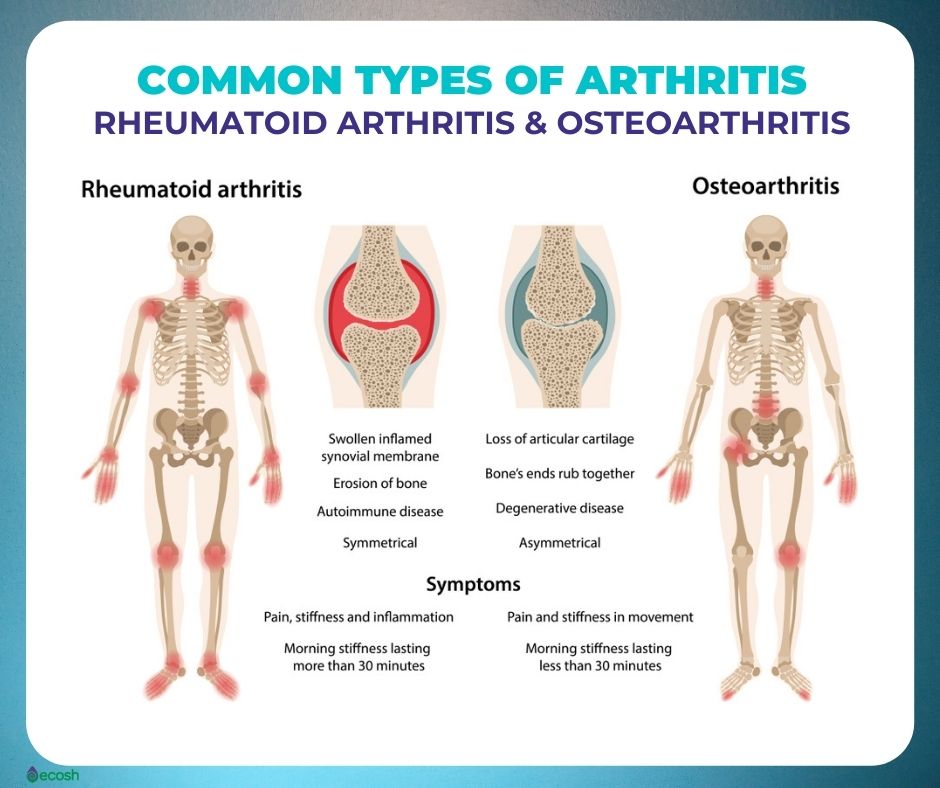
Arthritis Types
- Osteoarthritis. The most frequent type of arthritis that happens when the cartilage that cushions the ends of bones in your joints gradually degenerates.
- Rheumatoid arthritis. A kind of inflammatory arthritis, known as an auto-immune health condition.
- Gout and calcium crystal diseases. A kind of inflammatory arthritis that can typically affect the big toe. But it can also affect other joints in the body, and cause painful swelling.
- Spondyloarthritis. Spondyloarthritis is a word used to describe a number of conditions that cause pain and swelling, mainly around the joints of the spine. In these conditions there is inflammation of small pieces of connective tissues (entheses)
- Ankylosing spondylitis. A kind of spondyloarthritis that causes swelling and pain, mainly around the joints of the spine.
- Psoriatic arthritis. Psoriatic arthritis is a type of spondyloarthritis, and also an auto-immune condition that can cause painful stiffness and swelling within and around joints, as well as psoriasis (red scaly skin rash).
- Juvenile idiopathic arthritis (JIA). If someone is diagnosed with inflammatory arthritis before their sixteenth birthday, it’s called juvenile idiopathic arthritis, or JIA (2).
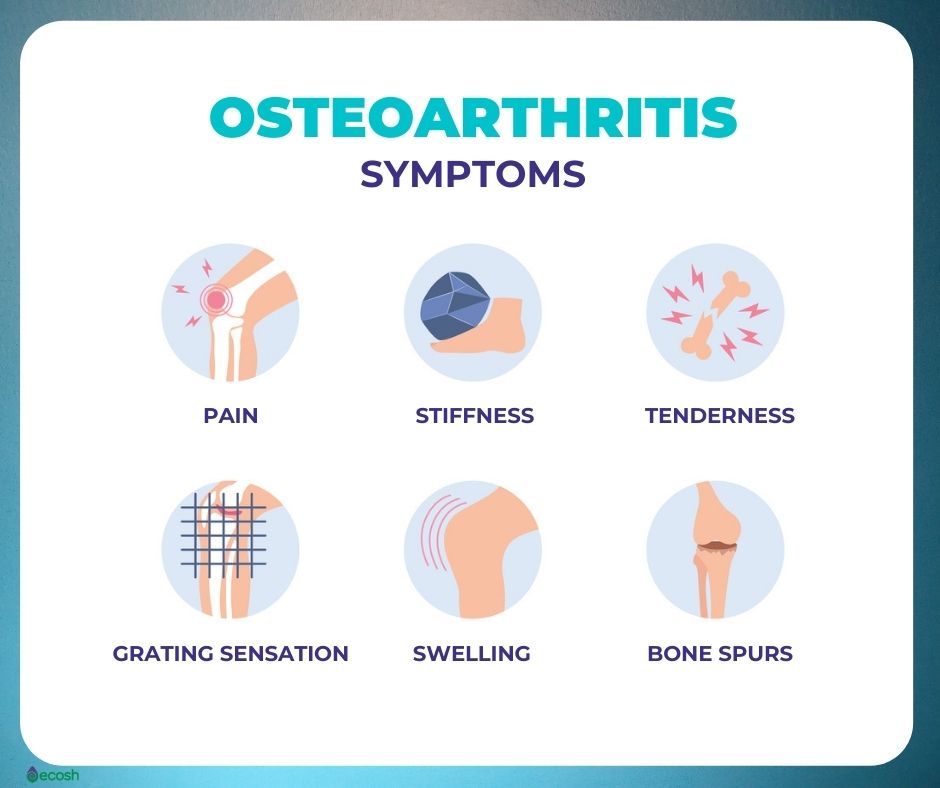
Osteoarthritis Signs and Symptoms
Usually osteoarthritis symptoms develop slowly and get worse over time. You may also notice that symptoms may vary for no obvious or vary depending on what you’re doing. If you have stiffness or joint pain that doesn’t go away, make an appointment and consult with your doctor. Signs and symptoms of osteoarthritis include:
- Stiffness in the affected joints. The stiffness might be most notable after awakening or being inactive. Your joints may feel stiff after awakening or being inactive. However, this mostly wears off quite quickly after moving.
- Pain in the affected joints. Pain is usually worse when you move the joint or at the evenings
- Tenderness in your joints. When you apply light pressure to your joint or near it, your joint might feel tender
- Loss of flexibility in your joints. Your joint may not move through its full range of motion.
- Grating, crackling or popping sounds and sensations. You might feel a grating, crackling or popping sensations and sounds as you move your joints (called crepitus).
- Bone spurs. Around the affected joint you may notice extra bits of bone, which feel like hard lumps.
- Thin or wasted muscles around the joint. Occasionally the muscles surrounding your joint may seem wasted or thin.
- Swelling. The affected joint may sometimes be swollen, which might be caused by soft tissue inflammation around the joint. The swelling may be:
- Weather and Diet. These factors may affect the symptoms of osteoarthritis, but aren’t a direct cause of it:
- Weather. According to many osteoarthritis patients, changes in the weather may make the pain worse, particularly when the atmospheric pressure is falling. Which happens for example, just before it rains.
- Diet. Some individuals have noticed that certain foods seem to lessen or increase their pain and other symptoms. However, your body weight is more likely than any other specific dietary factors to affect your risk of developing osteoarthritis (1, 4).
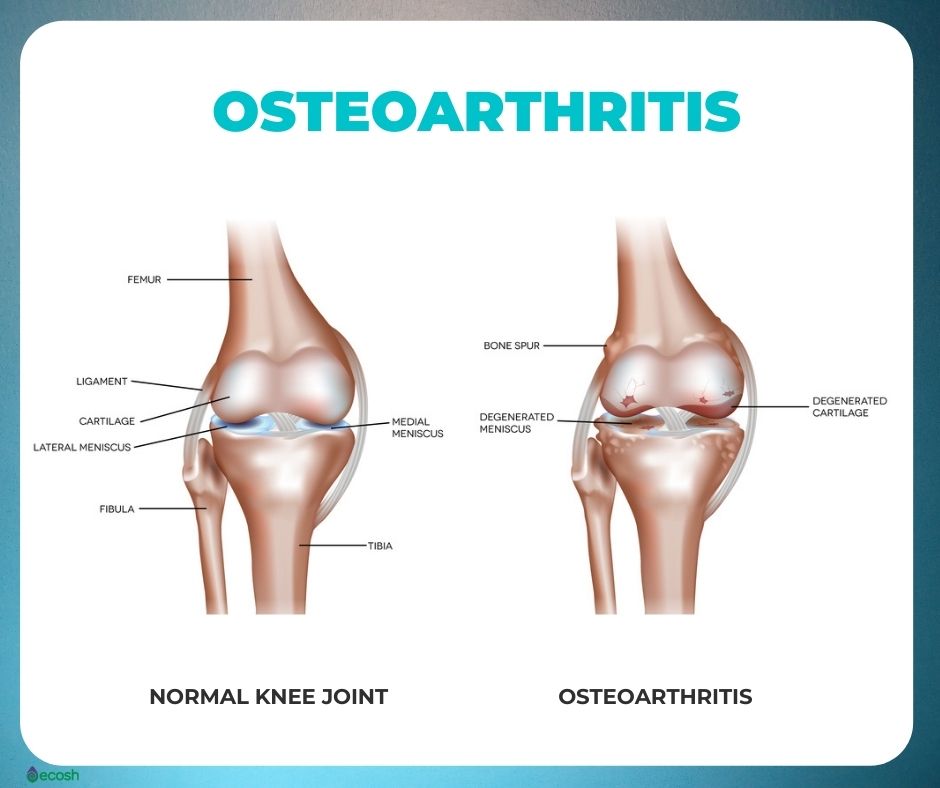
Osteoarthritis Causes
Osteoarthritis has mostly been spoken about as a “wear and tear” disease, and it’s still not entirely clear what causes it. It happens when the cartilage gradually degenerates. Cartilage is a dense and slippery tissue that enables untroubled and slick joint movement.
Finally, in case osteoarthritis, if the cartilage wears down entirely, bone will rub on bone.
Along with the breakdown of cartilage, this condition influences the entire joint. Osteoarthritis also causes degeneration of the ligaments – connective tissues that hold the joint together (as well as attach muscle to bone), and changes in the bone. In addition, it also causes inflammation of the joint lining (1, 2, 3).
Osteoarthritis Risk Factors
Osteoarthritis risk factors include:
Age. The risk of developing osteoarthritis grows with age, as it usually starts from the late 40s onwards. This may be because of the changes your body goes through due to ageing, such as weakening muscles and weight gain. Also the fact that your body becomes less able to heal itself effectively.
Gender. Osteoarthritis is usually more frequent and serious in women.
Obesity. Carrying more body weight puts stress to weight-bearing joints, for instance your hips and knees. Furthermore, fat tissue creates proteins that can cause harmful inflammation in and around your joints.
Joint injuries. A major injury that occurs when playing sports or from an accident, or operation on a joint may increase the risk and lead to osteoarthritis in that joint later in life.
Joint abnormalities. Some individuals are born with joint abnormalities or develop them in childhood. This may cause more serious and earlier osteoarthritis than usual.
Other types of joint disease. Occasionally osteoarthritis can be a result of damage from a different kind of joint disease, such as for example rheumatoid arthritis or gout.
Repeated stress on the joint. Normal activity and exercise don’t cause osteoarthritis, however extremely intensely, monotonous activity or physically difficult jobs may grow your risk. Therefore, if a physical exercise or your job places repetitive tension on a joint, that joint might finally develop osteoarthritis.
Genetic factors. Some people inherit the genes that can influence the risk of getting osteoarthritis at the hand, knee or hip. Few extremely rare forms of osteoarthritis are associated with mutations of single genes that influence collagen. This may cause osteoarthritis to develop in many joints at an earlier age than usual.
Bone deformities. Borning with malformed joints or defective cartilage may increase the risk of osteoarthritis.
Certain metabolic diseases. Conditions such as diabetes and hemochromatosis (a condition in which your body has too much iron) may also increase the risk (1, 4).
Osteoarthritis Prevention
Although it is not possible to prevent osteoarthritis completely, you may be able to lessen your risk of developing this disease by keeping up a healthy lifestyle and avoiding injuries.
- Exercise. Aim at least 150 minutes of modest aerobic exercise every week together with strength exercises (that work the major muscle groups) on 2 or more days each week. Try exercises such as cycling, fast walking and swimming, where the tension on your joints is more controlled, as exercises such as running and weight training put excessive pressure on your joints (5).
- Work on your posture. Avoid staying in the same position for too long and maintain good posture at all times (5).
- Lose weight. Being overweight increases the tension on your joints and your chance of developing osteoarthritis. Therefore, in case you are overweight, losing weight may help lessen your risk. Use a BMI calculator to find out whether you’re in normal weight, overweight or obese (5).
Osteoarthritis Treatment
Although osteoarthritis is irreversible, according to Mayo Clinic, treatments can reduce pain and help you move better (11).
Conventional Treatment for Osteoarthritis
- Medications that can help relieve primarily pain, include:
- Acetaminophen
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Duloxetine (Cymbalta)
- Therapy:
- Physical therapy
- Occupational therapy
- Procedures such as:
- Cortisone injections
- Lubrication injections
- Realigning bones
- Joint replacement
- Surgical and other procedures:
- Knee osteotomy
- Artificial hip
- Knee comparisons (11).
Lifestyle Changes, Alternative Medicine and Home Remedies for Osteoarthritis
Exercise. It’s important to strengthen the muscles around your joint, as it makes your joint more stable. Try walking, bicycling or water aerobics. If you feel new joint pain, stop and try again a day or two later at a lower level of intensity. See exercises for osteoarthritis here.
Lose weight. Even minor weight loss may relieve some pressure on your weight-bearing joints and reduce your pain.
Movement therapies. Research suggests that tai chi and yoga which involve gentle exercises and stretches combined with deep breathing might reduce osteoarthritis pain and improve movement.
Heat and cold. Heat, particularly moist heat, may help muscles relax and ease pain. Cold may reduce muscle spasms and lessen muscle pain after exercise.
Capsaicin. Topical capsaicin, a chili pepper extract might help some people when applied to skin over an arthritic joint.
Right footwear, braces or shoe inserts. Shoe inserts or other devices can support your joint to help take pressure off and therefore help reduce pain when you stand or walk.
Assistive devices. Assistive devices such as a cane or gripping and grabbing tools may help relieve stress on your joints or make it easier to work in the kitchen if you have osteoarthritis in your fingers.
Posture. Good posture may help to put less strain on your joints.
Pacing yourself. If you are doing a job that repeatedly increases your pain, try to break it down, allow yourself time for rest breaks, learn to pace yourself, and rotate with jobs that you find more effortless.
Transcutaneous electrical nerve stimulation (TENS). This provides short-term relief for some people with knee and hip osteoarthritis.
Acupuncture. Some studies indicate that acupuncture may relieve pain and improve function in people who have knee osteoarthritis. During acupuncture, hair-thin needles are inserted into your skin at precise spots on your body (2, 11).
However, talk to your dietician, doctor or movement instructor before practicing any self medication, exercise or starting any diet and taking any supplements.

6 Nutritional Supplements for Arthritis
According to the Arthritis Foundation, some supplements have shown promise for relieving pain, stiffness and other arthritis symptoms, especially when you use them together with traditional treatments. Listed nutritional supplements below are just some of the products researchers have studied for osteoarthritis (OA) and rheumatoid arthritis (RA) (6).
Glucosamine and Chondroitin. Although glucosamine and chondroitin are two components of cartilage—the substance that cushions the joints, the study results on these supplements have been mixed. This may be partly due to the fact that studies have used varying designs, types and supplements forms. Some evidence suggests glucosamine sulfate is best while others find glucosamine hydrochloride to be more effective. According to Mayo Clinic, evidence supports trying glucosamine sulfate for osteoarthritis of the knee (6, 7, 11).
Omega-3 fatty acids. These fatty acids have strong anti-inflammatory properties. According to Chris D’Adamo, PhD, director of Research & Education at the University of Maryland School of Medicine Center for Integrative Medicine – these fatty acids seem to work better for rheumatoid arthritis than for osteoarthritis, and this might be due to fact that rheumatoid arthritis is mainly driven by inflammation. When you take fish oil, make sure the supplement lists the EPA and DHA (the long-chain omega-3 fatty acids) content, as these have the majority of the health benefits (6, 11).
S-adenosyl-methionine (SAM-e). This natural anti-inflammatory compound in the body has also cartilage-protecting, and pain-relieving effects (6).
Curcumin. Curcumin is the active compound in the turmeric. In your body, curcumin acts as a strong anti-inflammatory agent. Although more research is still needed, current scientific evidence supports the effectiveness of turmeric extract (about 1000 mg/day of curcumin) in the treatment of arthritis (6, 8, 9, 10). Read more about the 22 scientifically proven health benefits of turmeric and curcumin.
Vitamins. Although so far there’s no scientific evidence that taking vitamins improves arthritis symptoms, vitamins D and K are both vital for bone strength, and vitamin K is included in cartilage structure. Therefore, taking these two vitamins may be helpful if you’re deficient in them (6). Read more about the health benefits of vitamin D and vitamin K.
Avocado-soybean unsaponifiables. This mixture of avocado and soybean oils acts as an anti-inflammatory agent, and according to some studies have shown to slow or even prevent joint damage (11).
However, do not start to self medicate and consult with your doctor before taking any nutritional supplements, as some of them may cause side effects or interact with the medicines you take. Read more about the research on the glucosamine, omega-3 fatty acids, SAM-e, curcumin and vitamins in the Arthritis Foundation page.

Complications, Coping and Support
Osteoarthritis is a disease that worsens over time. Joint pain and stiffness can become serious and cause difficulties to cope with daily life, depression and sleep disturbances.
Your capability to cope regardless of pain and disability caused by osteoarthritis often determines how much of an influence osteoarthritis will have on your daily life. Consult with your doctor if you’re feeling helpless, as there are several ways to relieve the problems osteoarthritis causes, and together you will find the most suitable remedy for you.
NB! The information provided here is for informational purposes only, so do not consider it as health care or medical diagnosis and treatment. Do not consider this information as a guarantee of the results you want to achieve. In addition, this information here is not intended to replace the advice of your physician or other healthcare professional.
Even more, you should not use it to diagnose or treat a health problem. Before changing or discontinuing your existing medication, treatment, or care, or taking any dietary supplements, be sure to consult with your healthcare professional or doctor before starting any diet or program, or if you suspect you may have a medical condition.
Compiled by Maria-Helena Loik
Pictures: Pexels.com, Pixabay.com, Shutterstock.com
Sources:
- Osteoarthritis – Symptoms and causes – Mayo Clinic
- Arthritis | Causes, symptoms, treatment | Versus Arthritis
- Cartilage – Wikipedia
- Osteoarthritis (OA) | Causes, symptoms, treatments (versusarthritis.org)
- Osteoarthritis – NHS (www.nhs.uk)
- Vitamins and Supplements for Arthritis
- Glucosamine – Mayo Clinic
- Curcumin among best supplements for osteoarthritis pain (chiroeco.com)
- Bio-optimized Curcuma longa extract is efficient on knee osteoarthritis pain: a double-blind multicenter randomized placebo controlled three-arm study | Arthritis Research & Therapy | Full Text (biomedcentral.com)
- Efficacy of Turmeric Extracts and Curcumin for Alleviating the Symptoms of Joint Arthritis: A Systematic Review and Meta-Analysis of Randomized Clinical Trials (nih.gov)
- Osteoarthritis – Diagnosis and treatment – Mayo Clinic