Fibromyalgia (FM), also called fibromyalgia syndrome (FMS), is a long-term medical condition that mainly affects the central nervous system and causes widespread musculoskeletal pain all over the body. Other accompanied symptoms include fatigue, sleep problems, mood issues and troubles with memory.
Individuals with fibromyalgia may also suffer from tension headaches, depression, anxiety, temporomandibular joint (TMJ) disorders, and irritable bowel syndrome (IBS).
These symptoms may gradually accumulate over time with no single triggering event, however often the trigger is some kind of traumatic event, such as surgery, infection, physical trauma, infection or significant psychological stress.
One of the main theories is that that repeated nerve stimulation causes the brain and spinal cord of people with fibromyalgia to change, and they have developed changes in the way the central nervous system (brain, spinal cord and nerves) processes the pain messages carried around the body (1, 31).
Although there is no cure for FM, some medications can help manage symptoms. In addition, exercise, relaxation, stress-managing measures and certain supplements may also may help (1).
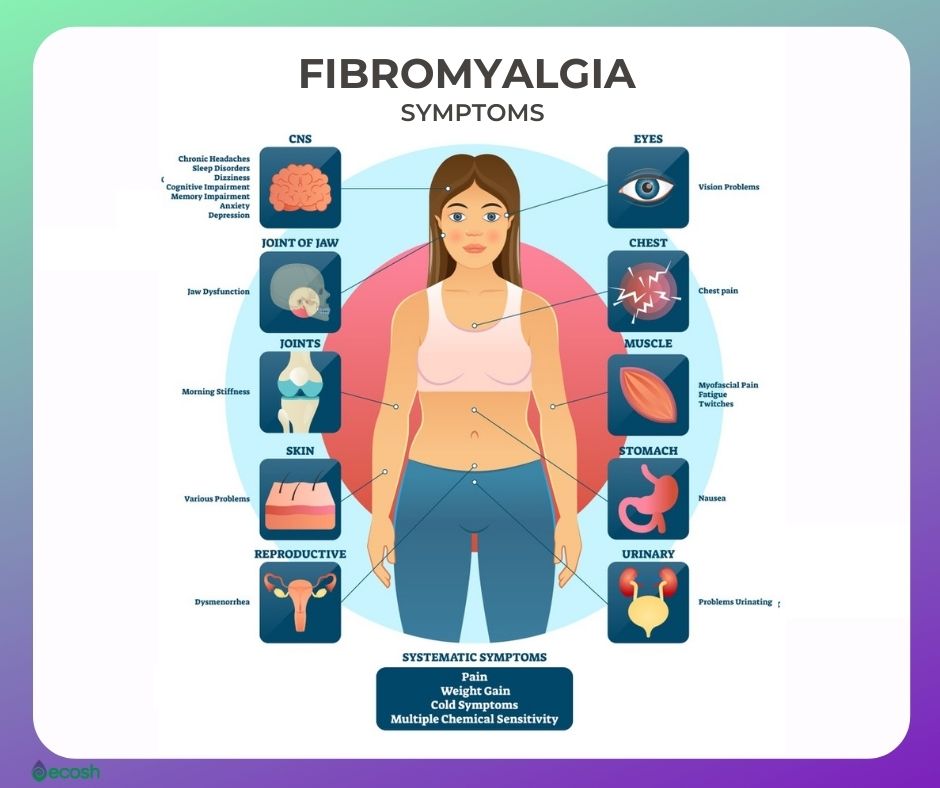
Fibromyalgia Symptoms
The symptoms of fibromyalgia mainly include:
Pain all over the body (widespread pain). Pain is usually described as a persistent dull ache which has lasted for at least three months, although it may be better or more severe at different times. The pain could also feel like a burning sensation or a sharp, stabbing pain. Widespread pain means that the pain occurs above and below your waist and on both sides of your body. You may feel the pain throughout your body, but it could be more severe in certain areas, such as your neck or back.
Stiffness. The stiffness may be most severe when you have been in the same position for a long period of time – for example, when you first wake up in the morning. Stiffness may also lead to muscle spasm.
Fatigue and tiredness. People with FM may often feel tired, even extremely tired (fatigue) or exhausted like often experienced during flu-like illness, even though they report sleeping for long periods of time.
Sleep problems. Pain may often disrupt your sleep, and many people with FM have other sleep disorders, for instance sleep apnea and restless legs syndrome. You may often wake up tired, even when you have had plenty of sleep, because the condition can sometimes prevent you sleeping deeply enough to refresh you properly. This is often described as non-restorative sleep.
Extreme sensitivity. This condition can make you very sensitive to pain all over your body, and even the slightest touch (such as stubbing your toe) might be painful. The pain also may last longer than it commonly would. In addition, being exposed to something you’re sensitive to (for example certain foods, bright lights, smoke) can cause your other fibromyalgia symptoms to flare up.
Cognitive difficulties (usually referred to as “fibro fog”). Problems with thinking, memory, remembering and learning new things, ability to focus, paying attention, concentrating on mental tasks or even slowed or confused speech.
Headaches, including migraines. These can range from being mild headaches to severe migraines, and could also include other symptoms, such as feeling sick.
Symptoms may also include tingling (pins and needles, known as paraesthesia), prickling, burning sensations or numbness in hands and feet.
Sometimes pain in the face or jaw, including disorders of the jaw known as temporomandibular joint syndrome (also known as TMJ).
Digestive problems, such as abdominal pain, bloating, and constipation.
Depression and anxiety.
Some other symptoms that individuals with FM sometimes undergo include clumsiness and dizziness, feeling too cold or too hot, an overwhelming urge to move your legs (restless legs syndrome), and in women, uncommonly painful periods.
- Fibromyalgia often coexists with other conditions, such as irritable bowel syndrome (IBS), chronic fatigue syndrome, interstitial cystitis or painful bladder syndrome, temporomandibular joint disorders, postural tachycardia syndrome (1, 2, 3).
Fibromyalgia Causes
The exact cause of fibromyalgia is not clear, but it’s likely that a number of factors are involved. Some of the main factors thought to contribute to FM:
Genetics. As fibromyalgia tends to run in families, genetics may play a part in the onset of this condition, with some people perhaps more likely than others to develop FM because of their genes. If this is the case, genetics could explain why many people develop fibromyalgia after some sort of trigger or life event (1, 3).
Physical or emotional events. Occasionally, FM can be triggered by a stressful event, including physical stress or prolonged emotional (psychological) stress. Possible triggers may be life events such as an injury, a viral infection, a car accident, giving birth, having an operation, the breakdown of a relationship, being in an challenging relationship, or the loss of a loved one (1, 3).
Infections. Some illnesses or viral infections seem to trigger or aggravate fibromyalgia (1, 3).
Abnormal pain messages. One of the main theories is that that repeated nerve stimulation causes the brain and spinal cord of people with FM to change, and they have developed changes in the way the central nervous system (brain, spinal cord and nerves) processes the pain messages carried around the body. This change involves changes in levels of certain chemicals in the brain that signal pain (1, 3).
Chemical imbalances. According to researchers, people with fibromyalgia have unusually low levels of the hormone serotonin in their brains, and they have abnormal dopamine response to pain. Low levels of these hormones may be a key factor in the cause of FM, as they’re important in regulating things like mood, appetite, sleep, behaviour, your response to stressful situations. These hormones also participate in processing pain signals sent by the nerves (1, 3, 29, 30).
Stress. Changes in the levels of some other hormones, such as for example cortisol, may also contribute to fibromyalgia. Cortisol is released when the body suffers from stress (1, 3).
- Sleep problems. Fibromyalgia may impede sleeping deeply and therefore lead to severe tiredness (fatigue). People with FM who sleep badly may also experience higher levels of pain. However, disrupted sleep patterns may not be just a symptom of fibromyalgia, it may possibly be a cause (1, 3).
Fibromyalgia Risk Factors
Risk factors include:
Gender. Fibromyalgia occurs more often in women than in men.
Family history. If your parent or sibling has FM, you may be at higher risk to also develop this condition.
Other disorders such as lupus, rheumatoid arthritis or osteoarthritis. If you have lupus or rheumatoid arthritis (RA), or osteoarthritis (OA) you are more likely to develop fibromyalgia.
Age. Although fibromyalgia may affect people of all ages, including children, most people are diagnosed during middle age the risk increases as you get older.
- In addition, also some other factors have been linked with fibromyalgia, but more research is needed to see if they are real. These possible risk factors include:
Diagnosis
To diagnose fibromyalgia, certain criteria generally have to be met. In addition to the patient’s history, physical examination, X-rays, and blood work, the most commonly used criteria for diagnosis are:
- You suffer from severe pain in 3 to 6 different areas of your body, or you suffer from milder pain in 7 or more different areas.
- The symptoms have continued at a similar level for at least 3 months.
- There has been found no other reason for your symptoms.
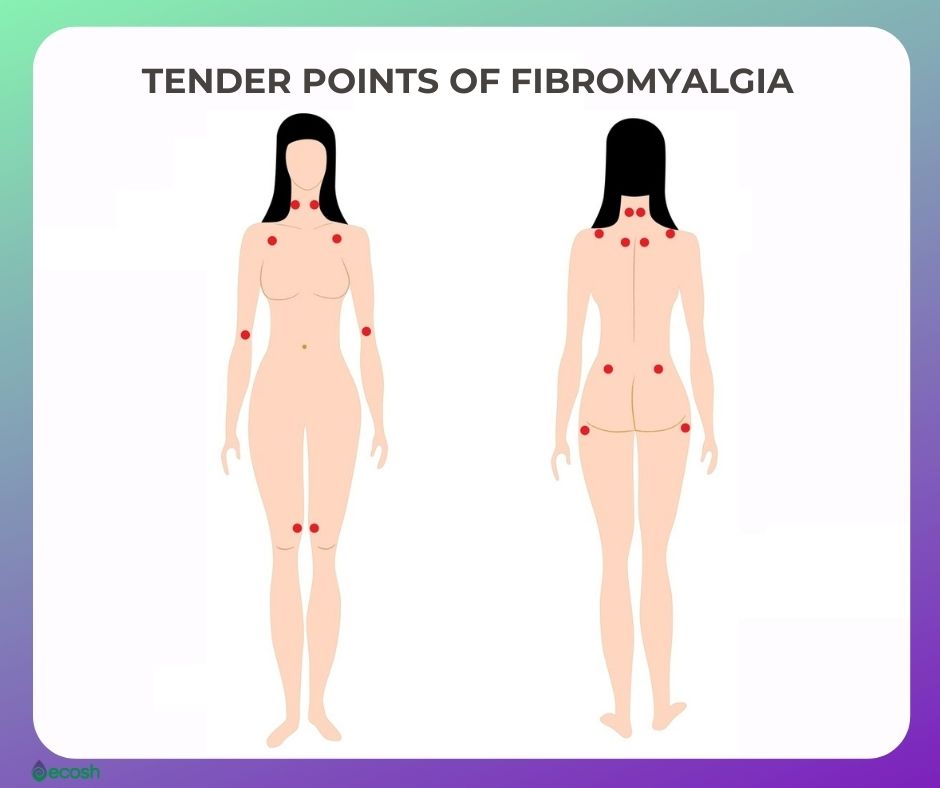
- The level of the pain used to be evaluated by applying tender pressure to certain areas called “tender points”. However, nowadays this method is less common (3).

Associated Conditions
There are several other conditions which are frequently associated with fibromyalgia. Therefore, before diagnosing fibromyalgia your doctor may first want to rule out certain conditions that may have similar symptoms such as:
- Osteoarthritis (OA)
- Lupus
- Rheumatoid arthritis (RA)
- Ankylosing spondylitis
- Temporomandibular disorder (TMD)
- Chronic fatigue syndrome (also known as ME)
- Multiple sclerosis (MS)
- Polymyalgia rheumatica
- Axial spondyloarthritis
- Thyroid disease
- Diabetes
- Anemia (3, 31, 32).
Fibromyalgia Treatment
Usually treatments for fibromyalgia include both medication and self-care strategies, as one treatment may not work for all symptoms. Therefore trying a selection of treatment methods can have a progressive effect (1).
Conventional Medicine – Medications for Fibromyalgia
Common medications that can help lessen pain and improve sleep include:
- Pain relievers. For example acetaminophen, ibuprofen or naproxen sodium. Opioid medications are not recommended, as these may cause significant side effects.
- Antidepressants. For example, duloxetine and milnacipran.
- Anti-seizure drugs. For example gabapentin or pregabalin (1).

Therapies, Alternative Medicine, Lifestyle and Home Remedies for Fibromyalgia Treatment
Self-care is critical in the management of fibromyalgia. Several different therapies, lifestyle and home remedies may help reduce the impact that fibromyalgia has on your body and daily life.
Stress management and counseling. Firstly, try to find some quiet place and allow yourself time to relax each day. Make up some plan on how to limit emotional stress without changing your routine completely, as individuals who drop all activity or quit work tend to do worse than do those who remain active. You can try some stress management techniques, such as meditation or deep-breathing exercises. Talking with a counselor may also be helpful (1, 7, 9).
Exercising regularly and physical therapy. Although exercising may firstly increase your pain, doing it regularly may often lessen the symptoms of fibromyalgia. Suitable exercises may involve water aerobics, stretching, walking, swimming and biking. Good posture and relaxation may also be important. A physical therapist can help you develop a home exercise program and teach you exercises that will improve your strength, flexibility and stamina (1).
Occupational therapy. An occupational therapist may help you make changes in some areas that may cause stress on your body, such as simple adjustments to your work place or the way you perform certain tasks (1).
Sleeping habits. Getting enough good quality sleep is vital in case of fibromyalgia. Try to sleep enough and practice good sleep habits like for example getting up and going to bed at the same time every day (1).
Pace yourself and do not push yourself too hard. Doing too much on good days, may lead to having more bad days. Therefore, try to find balance and plan your activity evenly. In other words, not doing too little on the bad days and not overdoing on good days.
Acupuncture. Although acupuncture, a Chinese medical system may not suit everyone, there is some evidence that it might help relieve fibromyalgia symptoms (1, 5, 6, 7).
Massage. According to a small study, massage therapy may have immediate beneficial effects on lessening pain, anxiety, and depression in people with fibromyalgia. Therefore, it might be one of the usable complementary and alternative treatments (1, 8).
Yoga and tai chi. According to studies, both may be helpful in managing fibromyalgia symptoms. (1, 9, 10).
- Maintain a healthy lifestyle. Eat healthy foods, limit caffeine, tobacco and alcohol, and do something pleasant each day (1).

Supplements for Fibromyalgia
Vitamin B12. Limited studies suggest that low B12 levels may be involved in chronic fatigue syndrome and fibromyalgia. In addition, methylcobalamin, which is a form of B12 has been shown to reduce chronic pain in fibromyalgia as well as in rheumatoid arthritis. Although the causes of both conditions are uncertain, the restoration of neuron cells is known to improve their symptoms (4, 11, 12, 21).
Minerals such as magnesium, calcium, copper, iron, and manganese. One study found that the concentrations of calcium, magnesium, iron, copper and manganese in the hair of female patients with fibromyalgia were lower than controls. If your blood test also reveals the deficiency of these nutrients, you may benefit from taking supplements or changing your diet (13, 14, 15, 16, 17, 21).
Vitamin D. Vitamin D deficiency also seems to be linked to fibromyalgia. Therefore, taking vitamin D supplements may improve the quality of life in patients with fibromyalgia (18, 19, 20, 21, 22).
Coenzyme Q10. This important substance has also shown some promise in lessening fibromyalgia symptoms such as pain and fatigue (21, 22, 23, 24, 25, 26).
Curcumin. According to several studies, Curcumin may be as effective as painkiller in relieving joint pain among rheumatoid arthritis and osteoarthritis patients. Therefore, if you are looking for natural pain killers, curcumin may be a worth to try (22, 27, 28).
NB! The information provided here is for informational purposes only, so do not consider it as health care or medical diagnosis and treatment. Do not consider this information as a guarantee of the results you want to achieve. In addition, this information here is not intended to replace the advice of your physician or other healthcare professional.
Even more, you should not use it to diagnose or treat a health problem. Before changing or discontinuing your existing medication, treatment, or care, or taking any dietary supplements, be sure to consult with your healthcare professional or doctor before starting any diet or program, or if you suspect you may have a medical condition.
Compiled by Maria-Helena Loik
Photos: Pexels.com, Pixabay.com, Shutterstock.com
Sources:
- Fibromyalgia – Symptoms and causes – Mayo Clinic
- Fibromyalgia | Arthritis | CDC
- Symptoms – Fibromyalgia – NHS (www.nhs.uk)
- Vitamin B12 May Help Treat Fibromyalgia – University Health News
- Fibromyalgia: Can acupuncture relieve symptoms? – Mayo Clinic
- Acupuncture therapy for fibromyalgia (nih.gov)
- Treatment of fibromyalgia with acupuncture and counseling| British Columbia Medical Journal (bcmj.org)
- Massage Therapy for Fibromyalgia (nih.gov)
- Managing fibromyalgia with yoga and meditation – PubMed (nih.gov)
- Tai Chi Has Similar or Greater Benefits Than Aerobic Exercise for Fibromyalgia | NCCIH (nih.gov)
- B12 for Fibromyalgia and Chronic Fatigue Syndrome (verywellhealth.com)
- Vitamin B12 and Fibromyalgia – Treating Fibromyalgia (techie.org)
- Women with Fibromyalgia Have Lower Levels of Calcium, Magnesium, Iron and Manganese in Hair Mineral Analysis (nih.gov)
- 6 Supplements for Fibromyalgia Symptom Relief (healthline.com)
- Magnesium, Melatonin, and Probiotics for Fibromyalgia (arthritis-health.com)
- Relation between magnesium and calcium and parameters of pain, quality of life and depression in women with fibromyalgia | Advances in Rheumatology | (biomedcentral.com)
- Magnesium Malate: Benefits, Side Effects, Dosage, and Interactions (verywellhealth.com)
- Vitamin D and fibromyalgia: a meta-analysis (nih.gov)
- Effects of Vitamin D Therapy on Quality of Life in Patients with Fibromyalgia (nih.gov)
- Vitamin D for Fibromyalgia (verywellhealth.com)
- Supplements — FIBROMYALGIA COALITION INTERNATIONAL (fibrocoalition.org)
- Turmeric, Vitamin D, and Coenzyme Q10 for Fibromyalgia (arthritis-health.com)
- Fibromyalgia symptoms improve with CoQ10 (medicalxpress.com)
- Q10 may help to treat fibromyalgia but also by treating underlying causes (healthandscience.eu)
- Effect of Oral Coenzyme Q10 Supplementation on Clinical Symptoms and Oxidative Stress in Fibromyalgia Patients: A Randomized Trial | (bmj.com)
- Fibromyalgia: Woman reversed symptoms | News | Pharma Nord UK
- Can Supplements Treat Fibromyalgia? Vitamin D, Turmeric, and More (webmd.com)
- Efficacy of Turmeric Extracts and Curcumin for Alleviating the Symptoms of Joint Arthritis: Meta-Analysis of Randomized Clinical Trials (nih.gov)
- Serum levels of serotonin as a biomarker of newly diagnosed fibromyalgia in women (nih.gov)
- FM patients show an abnormal dopamine response to pain – PubMed (nih.gov)
- Understanding Fibromyalgia and Its Related Disorders (nih.gov)
- FM Misdiagnosis: (creakyjoints.org)


