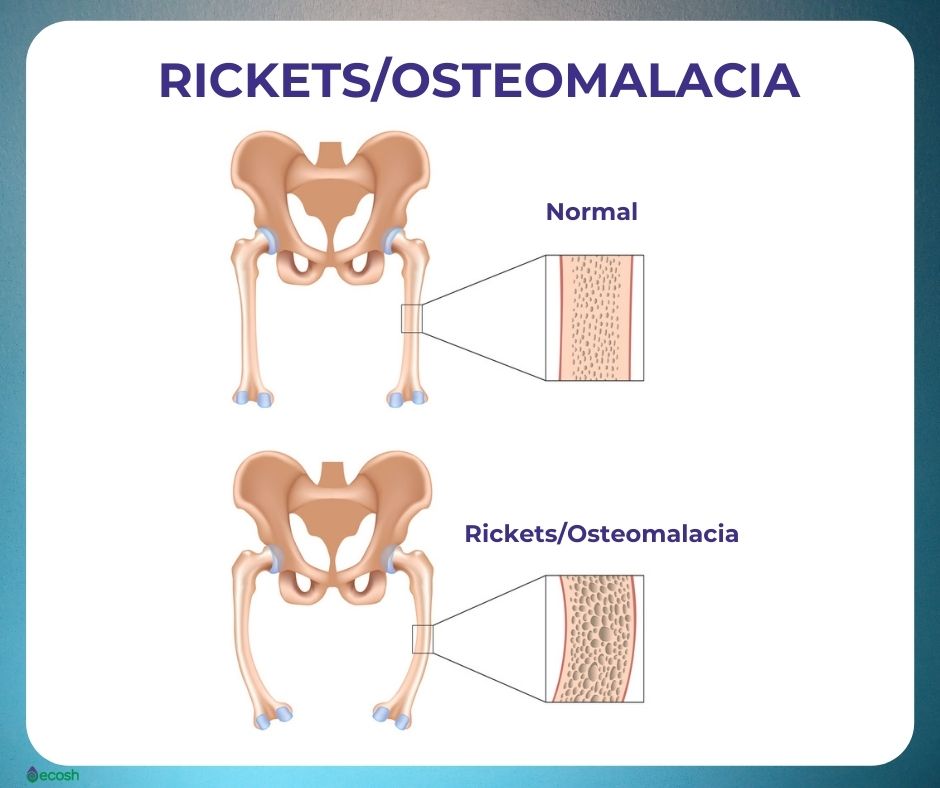
Osteomalacia is a bone condition characterized by defective mineralization of newly formed bones and softening of bones, which leads to bone weakening.
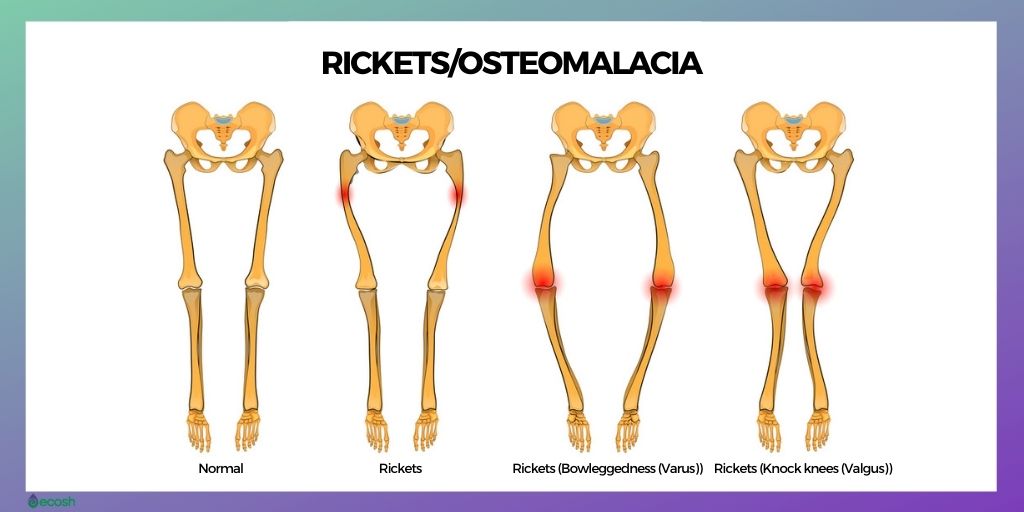
- In children and young adults this defective mineralization of the growing skeleton may lead to bending of the bones during growth (especially in weight-bearing bones of the legs), and cause permanent bone deformities (rickets).
- Defective skeletal mineralization in adults is known as osteomalacia, and in older adults osteomalacia may lead to fractures.
Osteomalacia, as well as osteopenia may not cause any symptoms in early stages. However, in later stages osteomalacia signs may include muscle weakness and spasms, bone pain, bone tenderness and difficulty walking. Both diseases increase the risk of breaking a bone.
As osteomalacia is caused by any condition (such as severe vitamin D deficiency) that results in inadequate calcium or phosphate mineralization of bone osteoid, its treatment mostly involves providing enough vitamin D and calcium, both required to harden and strengthen bones, and treating disorders that might cause the conditions (1, 2, 4, 12). By reading this article you will know more about osteopenia symptoms, causes, prevention and treatment.
Osteomalacia Symptoms
In its early stages, osteomalacia might not cause any symptoms, and the signs of osteomalacia might show on bone density or other diagnostic tests. However, when osteomalacia progresses, you might develop muscle weakness as well as bone pain. Osteomalacia symptoms may include:
- Needles and pins in feet and hands which is caused by low calcium levels
- Bone and joint pain
- A slight knock on a bone such as the shin may feel very painful
- Aching bone pain most commonly affects the lower back, groin, upper thighs, knees, pelvis, hips, legs and ribs
- You can feel the pain sometimes in the feet when you stand, walk or run, and it is rarely relieved completely by rest
- Muscle cramps
- Muscles may feel stiff
- Muscle weakness, the weakness tends to affect muscles in the thighs, shoulders and main part of the body – the trunk. Difficulties to climb stairs, get up from a chair without using the arms for support and, in very severe cases, get out of bed.
- Muscle pain, especially after exercise
- Waddling walk, as reduced muscle tone and leg weakness may make walking more difficult and slower
- Bones that break more easily from falls or simple knocks, particularly those in the hips, lower back and feet
- Lying down or sitting in order to rest often relieves the pain
- As the osteomalacia gets worse, you may feel the pain all over your body and simple movements can hurt
- Looser’s zones (partial fractures linked with osteomalacia), which may be extremely painful and make walking troublesome. Occasionally, these cracks can lead to full breaks, known as complete fractures (1, 3, 4).
Osteomalacia Causes
In short, osteomalacia is the result from a defect in the bone-maturing process. As everything else in your body, also bone is a living tissue, and old bone cells are constantly being removed and replaced with new cells (this process is called bone turnover). Bone has a hard outer shell (cortex), and soft and lighter structured inside (matrix).
The strength of the bones outer shell – which protects the softer inside – depends on how much layers of calcium and phosphorus are laid down, as these minerals form the outer shell and help build strong bones.
Therefore, if you don’t get enough of these minerals, you might develop osteomalacia. However, vitamin D has also plays a role in this process as it controls the levels of calcium and phosphorus in your body (1, 4).
In conclusion, if you don’t have sufficient amounts of calcium, phosphorus and vitamin D, your bones will become weak and soft (1, 4).
Osteomalacia can be caused by:
- Vitamin D deficiency. You do not get enough direct sunlight, eat vitamin D-rich foods, or vitamin D supplements (1).
- Kidney or liver disorders. As kidneys and liver play a role in activating vitamin D in your body, problems with these organs may influence your body’s ability to produce active vitamin D.
- Certain surgeries. If you have surgery to remove part or all of your stomach or to bypass your small intestine, it can cause calcium and vitamin D deficiency.
- Celiac disease. This autoimmune disease may lead to calcium and vitamin D deficiency, because damaged intestinal lining doesn’t absorb nutrients well.
- Medications. In addition, certain seizure medications, such as phenytoin and phenobarbital, may also lead to serious vitamin D deficiency and osteomalacia (1).

Osteomalacia Risk Factors and Risk Groups
The risk of developing osteomalacia is biggest in individuals who for several different reasons might not get enough vitamin D. As body produces vitamin D due to sun (UV light), gets it from vitamin D rich foods or supplements, the biggest risk groups for vitamin D deficiency are the elderly and people with reduced mobility and sedentary lifestyle. In fact, also with age, the body’s ability to produce vitamin D decreases significantly (1, 4).
- Pregnant women, breastfeeding women and children
- Individuals who wear clothing that covers a lot of their skin.
- Adults over 65 or when kidneys cannot convert vitamin D
- People who have limited exposure to sunshine like office workers, or individuals who are all ill to go outside
- People with darker skin
- Inflammatory bowel disease patients
- People with a high body fat percentage
- Vegans and vegetarians
- In addition, people with certain medical problems, including kidney failure, liver diseases, untreated coeliac disease, stomach surgery, Crohn’s disease, cystic fibrosis, and celiac disease, as these conditions may affect your intestine’s ability to absorb vitamin D from the food
- In conclusion, people taking certain medications which can all impair vitamin D metabolism:
It’s important to talk to your doctor if any of the above applies to you.

Osteomalacia Prevention
As osteomalacia is caused by vitamin D deficiency, it can be often prevented by getting adequate amounts of vitamin D (1, 4). Read more about other health benefits of vitamin D, and vitamin D rich foods.
Eat vitamin D-rich foods. Foods that contain the most vitamin D include cod liver oil, fatty fish (salmon, mackerel, sardines) and egg yolks. For example:
- Cod liver oil: 34.0 mcg (1,360 IU)/1 tbsp – 170% DV
- Trout (rainbow), farmed, cooked: 16.2 mcg (645 IU)/3oz – 81% DV
- Salmon (sockeye), cooked: 14.2 mcg (570 IU)/3 oz – 71% DV
- Mushrooms, white, raw, sliced, exposed to UV light: 9.2 mcg (366 IU)/ ½ cup – 46% DV
- Milk, 2% milkfat, vitamin D fortified: 2.9 mcg (120 IU)/1 cup – 15% DV
- Soy, almond, and oat milks, vitamin D fortified, various brands: 2.5-3.6 mcg (100-144 IU)/1 cup – 13-18% DV
- Ready-to-eat cereal, fortified with vitamin D: 2.0 mcg (80 IU)/1 serving – 10% DV
- Sardines (Atlantic), canned in oil, drained: 1.2 mcg (46 IU)/2 sardines – 6% DV
- Egg, scrambled (only yolk contains vitamin D): 1.1 mcg (44 IU)/1 large – 6% DV
- Liver, beef, braised: 1.0 mcg (42 IU)/3 oz – 5% DV
Get moderate amounts of sunlight. To maintain healthy vitamin D levels in your body, you should aim to get 10–30 minutes of midday sunlight, several times per week. In fact, people with darker skin may need even a little more than this. However, do not overdo, as too much sun exposure may increase your risk of getting skin cancer.
Exercise. Regular exercise is vital for healthy bones, and also in osteopenia and osteoporosis prevention.
Calcium. Although calcium deficiency is not a common sole cause of osteomalacia, it’s vital for strong bones. Good sources of calcium include:
- Green leafy vegetables like for example kale, spinach, turnips
- Canned salmon or fish with bones such as sardines
- Tofu, Soybeans and fortified soymilk
- Enriched breads, grains, and waffles
- Dried fruit
- Yoghurt
- Cheese
- Milk
- Fortified cereals
- Fortified orange juice
If needed, take supplements. If you suspect that you don’t get sufficient amounts of vitamins and minerals in your diet or if your digestive system does not absorb nutrients properly due to some medical condition, consult with your doctor about taking calcium and vitamin D dietary supplements (1, 8, 9, 10, 11, 13, 14, 15).
Osteomalacia Treatment
- If you have osteomalacia, which is basically the adult form of rickets that causes soft bones – usually the treatment with vitamin D supplements will cure the condition. However, although you will probably need to take vitamin D supplements every day for a long period- it may take several months before any muscle weakness or bone pain is relieved. Moreover, when you stop taking the supplements, or do not take these regularly – the osteomalacia may return.
- Calcium supplements may also escalate the bone healing process.
- People with kidney failure or inherited forms of osteomalacia may usually need special forms of vitamin D (for example calcitriol pills) and lifelong support from their doctor (4, 11).
NB! The information provided here is for informational purposes only, so do not consider it as health care or medical diagnosis and treatment. Do not consider this information as a guarantee of the results you want to achieve. In addition, this information here does not replace the advice of your physician or other healthcare professional.
Even more, you should not use it to diagnose or treat a health problem. Before changing or discontinuing your existing medication, treatment, or care, or taking any dietary supplements, be sure to consult with your healthcare professional or doctor before starting any diet or program, or if you suspect you may have a medical condition.
Compiled by Maria-Helena Loik
Photos and graphics: Pexels.com, Pixabay.com, Shutterstock.com
Sources:
- Osteomalacia – Symptoms and causes – Mayo Clinic
- Does Osteopenia Hurt? Causes, Treatment & Diet (medicinenet.com)
- Osteomalacia (Soft Bones): Symptoms, Causes, Treatments & Tests (clevelandclinic.org)
- Osteomalacia | Causes, symptoms, treatment | Versus Arthritis
- https://www.webmd.com/diet/guide/vitamin-d-deficiency#1
- https://www.prevention.com/health/a20488821/risk-for-vitamin-d-deficiency/
- https://www.prevention.com/health/a20488821/risk-for-vitamin-d-deficiency/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3356951/#:~:text=Vitamin%20D3%20(cholecalciferol)%20is,scientifically%20known%20as%2022%2Ddihydroergocalciferol.
- https://www.healthline.com/nutrition/vitamin-d-from-sun#dangers
- https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/
- Rickets and osteomalacia – Treatment – NHS (www.nhs.uk)
- Rickets & Osteomalacia | Current Medical Diagnosis and Treatment 2020 | AccessMedicine | McGraw-Hill Medical (mhmedical.com)
- https://www.mayoclinic.org/diseases-conditions/osteoporosis/symptoms-causes/syc-20351968
- https://www.nhs.uk/conditions/osteoporosis/prevention/
- https://www.webmd.com/food-recipes/features/10-calcium-rich-foods