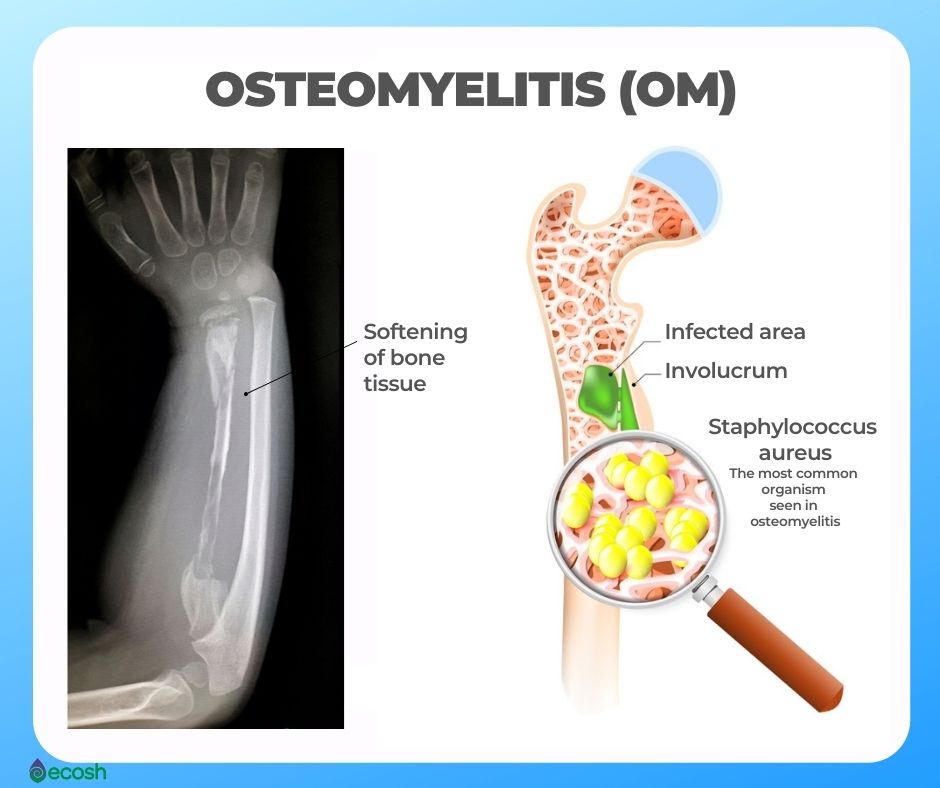
Osteomyelitis (OM) is a bacterial, or in rare cases a fungal infection of the bone which affects about 2 out of every 10,000 people. Bacteria can reach a bone by traveling through the bloodstream or spreading on from infected nearby tissue. Infections may also start in the bone itself if an injury uncovers the bone to germs.
If you leave the infection untreated, it can become chronic and lead to a loss of blood supply to the affected bone. When this occurs, it can eventually cause a death of the bone tissue. That is why it is extremely important to keep even the minor wounds clean.
In children, the long bones of the arms and legs are most commonly involved, while the spine, feet and hips are most commonly involved in adults. Treatment of bacterial osteomyelitis often includes both antimicrobials and surgery. Treatment of the relatively rare fungal osteomyelitis as mycetoma infections requires antifungal medications (1, 2, 4).
Osteomyelitis Signs and Symptoms
Onset of osteomyelitis may be sudden or gradual. Occasionally there might be no symptoms or the symptoms are hard to differentiate from other health conditions. Like for example in infants, older adults and individuals with compromised immune systems.
Common signs and symptoms of osteomyelitis may include:
- Fever
- Swelling, redness and warmth in the influenced area
- Pain and/or tenderness in the infected area
- Weakness
- Fatigue
- Irritability
- Enlarged lymph nodes may also be present
- Nausea, secondarily from being ill with infection
- Overall discomfort, feeling ill or uneasiness
- Drainage of thick yellow fluid (pus) through the skin
- Chills
- Difficulty walking on changes in walk (walking pattern that is painful, yielding a limp) or unwillingness to bear weight in children
- Other symptoms that may be linked with this disease include excessive sweating, lower back pain (if the spine is involved), loss or decline of movement of a joint, swelling of the ankles, feet, and legs (1, 2, 3, 4, 5).
Osteomyelitis Causes
Osteomyelitis can be caused by a range of microbial agents (most frequently by Staphylococcus, Pseudomonas, and Enterobacteriaceae) in situations when germs enter a bone, such as:
- Injuries:
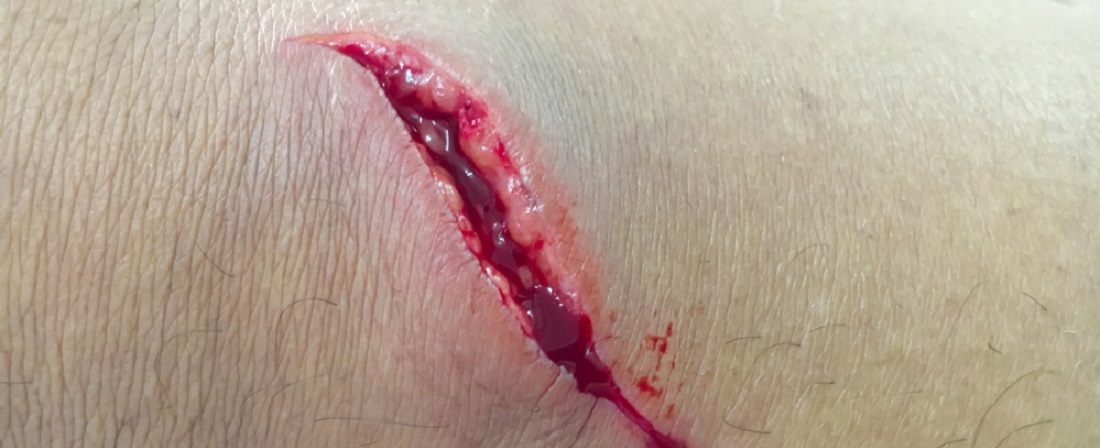
- Puncture wounds can transfer bad bacteria deep inside the body and these bad bacteria can spread into a nearby bone.
- Broken bone, such as an open fracture with the bone ends coming out through the skin.
- Surgery. Direct infection can occur during surgeries (for example to repair fractures or replace joints).
- A minor trauma. Trauma can cause a blood clot around the bone and lead to a secondary infection from seeding of bacteria.
- A chronic soft tissue infection or open wound may in the end spread down to the bone surface, which causes a direct bone infection.
- Bacteria in the bloodstream. Microbes in your body (for instance, germs in the lungs from pneumonia or in the bladder from a urinary tract infection) can travel through your bloodstream to a weakened spot in a bone. However, new bone often forms around the site (1, 3, 4).
Osteomyelitis Risk Factors and Risk Groups
Osteomyelitis may attack both adults and children. However, the fungus or bacteria that causes osteomyelitis, may be different among age groups. In children, osteomyelitis commonly affects the adjacent ends of long bones (bones in the arms or legs). In adults, osteomyelitis frequently affects the vertebrae and the pelvis (4).
Risk factors that can make your bones more vulnerable to osteomyelitis may include:
- Recent injury such as a severe bone fracture, deep puncture wound, an animal bite or a nail piercing through a shoe.
- Orthopedic surgery to repair broken bones or replace worn joints.
- Circulation disorders. When your blood vessels are blocked or damaged, your body has difficulties distributing the infection-fighting cells that are vital for keeping a tiny infection from growing larger. Health conditions that diminish blood circulation include:
- Poorly controlled diabetes
- Peripheral artery disease, often related to smoking
- Sickle cell disease
- Problems requiring intravenous lines or catheters. For example:
- Dialysis machine tubing
- Urinary catheters
- Long-term intravenous tubing, sometimes called central lines
- Conditions that damage the immune system. For example:
- Cancer treatment
- Poorly controlled diabetes
- Taking corticosteroids or tumor necrosis factor inhibitors
- Intravenous drug users in case they use non sterile needles and do not sterilize their skin before injections.
- The elderly. In general, bones are resistant to infection, however this protection decreases as people get older (1, 4).
Osteomyelitis Prevention
- If you suspect an increased risk of infection, consult with your doctor about methods to prevent infections from occurring, as lessening your risk of infection will also decrease your risk of developing osteomyelitis.
- It’s also important to take steps to manage any chronic conditions or unhealthy lifestyles you may have, such as keeping your blood sugar controlled if you have diabetes and quitting smoking.
- Boost your immune system and eliminate any inflammation in your body, as general inflammation in your body may make the infections worse and slow down the healing process. Together with a healthy lifestyle, also vitamin C supplements may help you to improve your immune function.
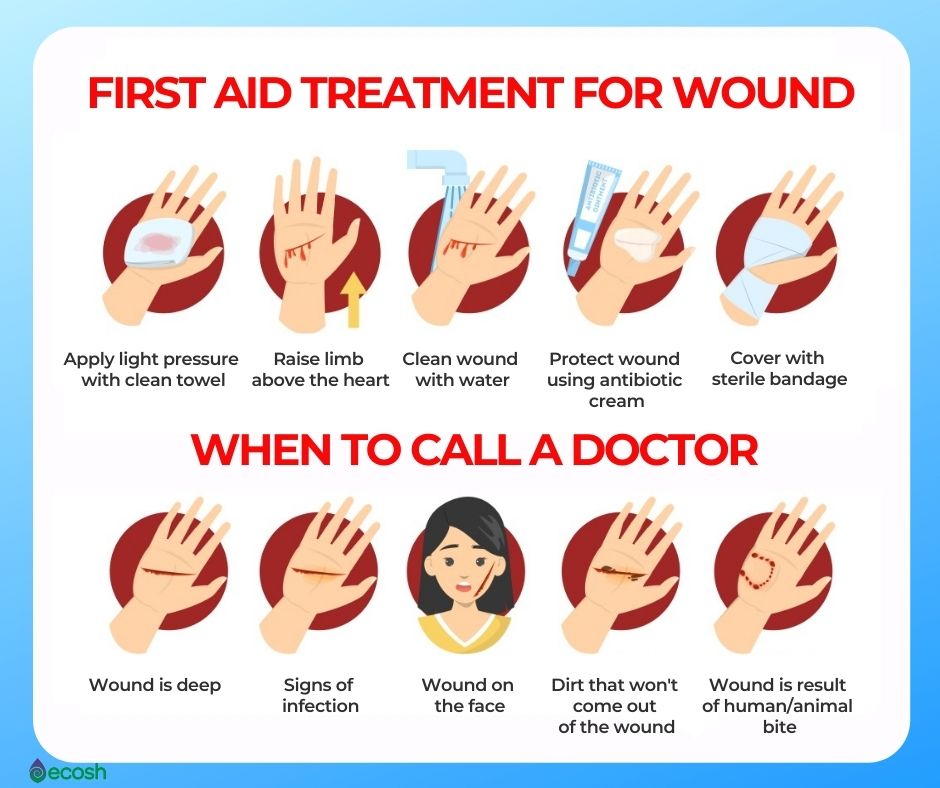
- Take precautions to avoid scrapes, cuts and animal scratches or bites, as these give bacteria easy access to your body.
- In case minor injury, clean the area of the injury immediately and apply a clean bandage.
- Check wounds frequently for signs of infection (1).
Osteomyelitis Treatment
- Medications. In numerous cases, antibiotics and pain medications successfully treat osteomyelitis, and a bone biopsy can help guide the choice of the best antibiotic. Fungal osteomyelitis requires antifungal medications (1).
- Drainage: In case there is an open wound or abscess, it may be drained through a procedure called needle aspiration, where a needle is placed into the infected area to withdraw the fluid (1, 4).
- Surgery. Surgery may include one or more of the following procedures:
- Draining the infected area. Opening up the area around the infected bone to drain the fluid.
- Removing diseased bone and tissue. Removing as much of the diseased bone (also surrounding tissue that shows signs of infection) as possible and taking a small margin of healthy bone to ensure that all the infected areas have been removed.
- Restoring blood flow to the bone. Filling any empty space left by the previous procedure with a piece of bone or other tissue, such as skin or muscle, from another part of your body or sometimes with temporary fillers.
- Removing any foreign objects. When foreign objects, like for example screws or surgical plates are placed during a previous surgery, these may have to be removed.
- Amputating the limb. Amputating the affected limb to stop the infection from spreading further (1).
NB! The information provided here is for informational purposes only, so do not consider it as health care or medical diagnosis and treatment. Do not consider this information as a guarantee of the results you want to achieve. In addition, this information here is not intended to replace the advice of your physician or other healthcare professional.
Even more, you should not use it to diagnose or treat a health problem. Before changing or discontinuing your existing medication, treatment, or care, or taking any dietary supplements, be sure to consult with your healthcare professional or doctor before starting any diet or program, or if you suspect you may have a medical condition.
Compiled by Maria-Helena Loik
Photos: Pexels.com, Pixabay.com, Shutterstock.com
Sources:
- Osteomyelitis – Symptoms and causes – Mayo Clinic
- Osteomyelitis – Wikipedia
- Medicinenet.com – Osteomyelitis Treatment, Symptoms, Definition & Causes (medicinenet.com)
- Osteomyelitis: Causes, Symptoms, Diagnosis & Treatments (clevelandclinic.org)
- Osteomyelitis: Symptoms, Causes, Diagnosis and More (verywellhealth.com)


